Every year, 100-200 people in the US contract leptospirosis, but usually 50% of the cases occur in Hawaii where outdoor adventurers are exposed to Leptospira bacteria found in freshwater ponds, waterfalls, streams, and mud. That's why it's so alarming that two people in the Bronx have been diagnosed with the disease and a 30-year-old man has died from it.
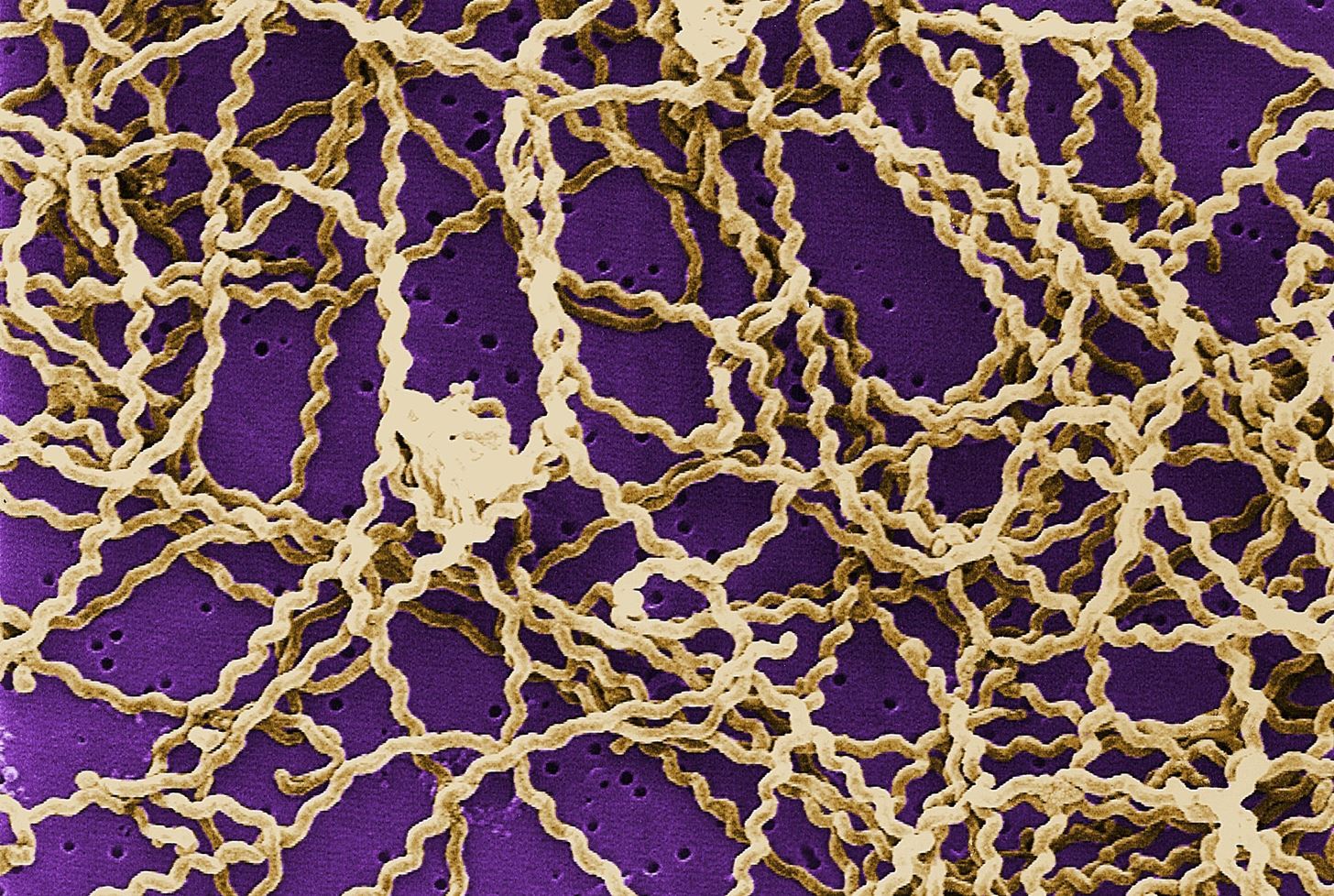
The bacteria that causes leptospirosis are a type called spirochetes and have the characteristic shape of a corkscrew. They are carried by animals—rats in the recent New York cases—who excrete the organism in their urine. If rats urinate in water, where the bacteria can survive for weeks or even months, there's a risk that it can be consumed by humans who drink or play in it.
Animal infections that are passed to humans, like this case, are called zoonotic infections. And leptospirosis is the most widespread zoonotic disease in the world.
However, only a few cases are reported in the state of New York each year—in people, that is. Dogs can catch leptospirosis, too. A study estimated 8% to 10% of dogs have leptospirosis antibodies, evidence of past infection.
Not all rats are infected with Leptospira bacteria, and those that are don't have symptoms of the illness. They may also be intermittent carriers. In an area of Baltimore associated with leptospirosis in human patients, 19 of 21 trapped rats showed evidence of carrying the bacteria.
Interestingly, the Centers for Disease Control and Prevention (CDC) stopped collecting data on US cases of human leptospirosis in 1994 for several reasons, including the fact that they had recorded a low incidence of 2 to 4 infections per 10 million people from 1985 to 1994. Since then, though, the CDC and the Council of State and Territorial Epidemiologists have changed their tune: Leptospirosis was reinstated in 2014 as a disease for which CDC must be notified.
Between 1999 and 2008, the infection rate had increased in the US to 163 to 285 infections per 10 million people, and we'd developed new technology to accurately confirm infections. New risk groups had been identified (30 triathletes in Illinois and Wisconsin were infected in 1998), and concern mounted that outbreaks might go unrecognized if not reported to a central agency.
The Disease in You & Your Dog
Some people infected with Leptospira have no symptoms, but others get fever, headache, chills, vomiting, jaundice (yellowing of the skin or whites of eyes), anemia, and sometimes a rash. Because these are pretty common symptoms, leptospirosis can easily be mistaken for other infections.
Antibiotics can cure leptospirosis, but in about 10% of people, the infection develops into more serious form called Weil's disease that can involve internal bleeding, kidney and liver failure, chest pain, coughing up blood, breathing problems, and brain damage. This severe type of leptospirosis is life-threatening and about 1% to 5% of people with Weil's disease die.
All three of the Bronx patients had severe illnesses and were hospitalized with acute kidney and liver failure, although the news reports did not name Weil's disease by name. Two of the patients also developed pulmonary hemorrhage, and one of those two died.
All three cases occurred within a one block radius of 750 Grand Concourse in the Bronx, and because of the rat infestation in the apartment where one victim lived, the source is suspected to be exposure to rat urine, according to a report by Dr. Mary Travis Bassett, the commissioner of the New York City Department of Health and Mental Hygiene. In the press conference video below, she recommended that anyone who lives in an area with a high rat population and experiences flu-like symptoms should see a physician.
Besides people who live in areas where rats may also be present, people who spend time outside are at the most at risk for getting leptospirosis. That includes farmers, sewer workers, veterinarians, fishers, aquaculturists, dairy farmers, and military personnel. It also includes "exposure events," where people come in contact with water contaminated with the organism, like during a flood or even when kayaking, rafting, and canoeing.
It's theoretically possible that leptospirosis could be passed from person to person if someone ingests or gets an infected person's urine in an open wound, but if it has happened, it's extremely rare. The bacteria is only excreted through the kidneys so other bodily fluids (like spit or semen) can't pass the infection on.

Leptospira organisms have been found in every species of mammal tested for it so far. In addition to rats, it's also found in dogs, cattle, and pigs. Domestic dogs can contract the disease much the same way as humans, and their symptoms are similar—fever, chills, vomiting, diarrhea, loss of appetite, lethargy, jaundice, or painful inflammation within the eyes.
There are canine vaccines available that cover four types of Leptospira organisms that dogs may come in contact with. Like rats and some people, dogs may act as carriers of bacteria and not get sick from the infection. Canine vaccinations can help to prevent the disease and the carrier status. That, in turn, decreases Leptospira shed in the dog's urine to infect others, including people.
Getting your dog vaccinated, avoiding contact with animal urine if you have cuts in the skin, and not swimming or walking in shallow water are all measures you can take to decrease your chance of catching leptospirosis.
We need to keep an eye on this reemerging infection. Take the steps you need to protect yourself and your dog against leptospirosis. And stay away from rats.
Just updated your iPhone? You'll find new emoji, enhanced security, podcast transcripts, Apple Cash virtual numbers, and other useful features. There are even new additions hidden within Safari. Find out what's new and changed on your iPhone with the iOS 17.4 update.





















Be the First to Comment
Share Your Thoughts