Streptococcus and staphylococcus bacteria produce toxins that can cause toxic shock syndrome.
Originally associated with infections related to tampon use, today more than half of the infections are due to other types of infection. Skin infections, burns, and surgical sites can all become infected with bacteria that can lead to toxic shock syndrome. While it's been around for awhile, it's still kind of a mystery why this infection is so dangerous. Scientists have just discovered a new way these infections become lethal.
A new study found that a type of immune cell that usually fends off pathogens, called mucosa-associated invariant T (MAIT) cells, can turn against us. In certain infections, this can cause severe disease and even death, according to the research, led by Mansour Haeryfar at Western University, in Canada.
The new research was published June 20 in PLOS Biology.
How Bacteria Cause Toxic Shock Syndrome
Toxic shock syndrome happens when bacterial toxins act as what the researchers have dubbed "superantigens", which cause an exaggerated and overwhelming immune response. While usually having your immune system respond to invaders is good, it's also deadly. Our body's immune response causes many of the symptoms of illness: Be it fatigue, fever, or snotty colds. Usually, these responses act to clear the invaders from our bodies, but sometimes they go into overdrive.
In the case of toxic shock, this overreaction of the immune system to these superantigen toxins means that large numbers of T cells release proteins called cytokines — a cytokine 'storm' — that causes fever, rash, shock, low blood pressue, and rapidly progressive multiple-organ failure. Toxic shock is even more devastating, because it often happens in young, previously healthy patients.
Patients are treated with intravenous antibiotics or intravenous immune globulins to try to kill the bacteria, and fluids to raise blood pressure. The trouble is that antibiotics are completely ineffective against toxins already in the blood system.
Thankfully, toxic shock syndrome is pretty rare. Streptococcal toxic shock syndrome occurs in about 3 per 100,000 people a year in the US, while the rate of toxic shock syndrome caused by staphylococcal infections is about 0.5 per 100,000 people annually.
Being relatively rare doesn't make it any less devastating. The death rate from staphylococcal toxic shock syndrome is about 4%, but nearly 40% of people who get streptococcal toxic shock syndrome die.
Getting to the cause of the devastation wreaked by toxic shock syndrome was an objective of the new research study by Haeryfar and his team.
MAIT Cells Turn Against Us
The researchers used animal models and human cells to show that MAIT cells hyper-respond when bacterial superantigens — toxins from strep or staph — are present. They also found that when MAIT cells respond to superantigens, they become worn out and eventually stop participating in a response aimed at killing the bacteria. When the immune response stops, the bacteria can thrive, leading to fatal consequences from the strep or staph, or increased susceptibility to other opportunistic infections, microbes that can infect more easily in a weakened immune system.
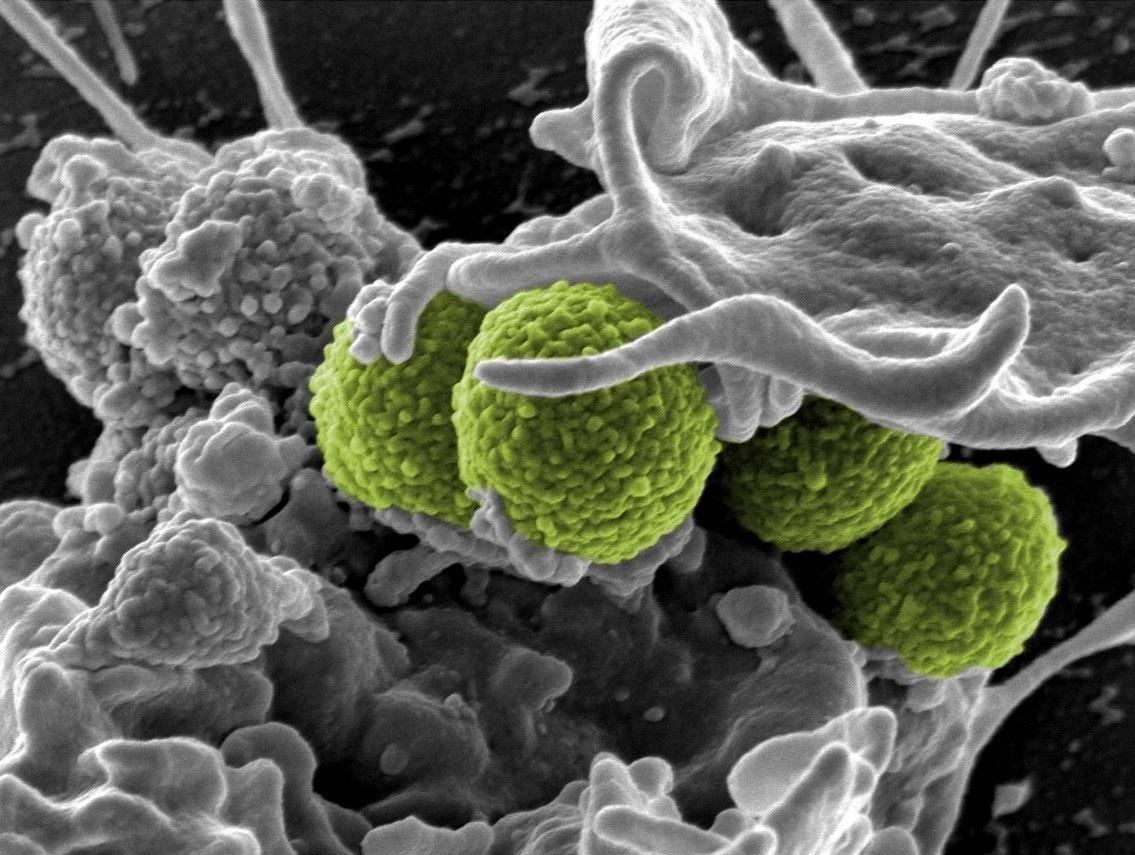
The new study revealed that MAIT cells might hold the key to the effects of the potentially-deadly cytokine storm created during toxic shock syndrome, and to why our bodies don't effectively get on top of the types of infections that cause toxic shock syndrome.
"Based on our findings, we propose that timely and efficient therapies that target MAIT cells will likely benefit the patients by preventing uncontrolled inflammation and also by relieving immunosuppression," Haeryfar said.
Just updated your iPhone? You'll find new emoji, enhanced security, podcast transcripts, Apple Cash virtual numbers, and other useful features. There are even new additions hidden within Safari. Find out what's new and changed on your iPhone with the iOS 17.4 update.




















Be the First to Comment
Share Your Thoughts