As unappealing as it sounds, transplants with fecal material from healthy donors help treat tough Clostridium difficile gastrointestinal infections. Researchers credit the treatment's success to its ability to restore a healthy bacterial balance to the bowels, and new research has shown that the transplanted bacteria doesn't just do its job and leave. The good fecal bacteria and its benefits can persist for years.
Researchers from the University of Alabama at Birmingham developed a method that could detect minute differences in microbes, allowing them to tell which bacteria came from the donor and which was a part of the transplant recipient. These bacteria make up the gut microbiome — the community of bacteria, viruses, and fungi that live in the gut and help us digest nutrients and keep us regular.
The study by first author Ranjit Kumar and colleagues was published online June 7 in npj Biofilms and Microbiomes.
The researchers' new method "will form the cornerstone of a personalized medicine approach to improve human health by providing an early warning system to detect disruption of the gut microbial community structure," co-author Casey Morrow said in a press release.
C. Diff Infections
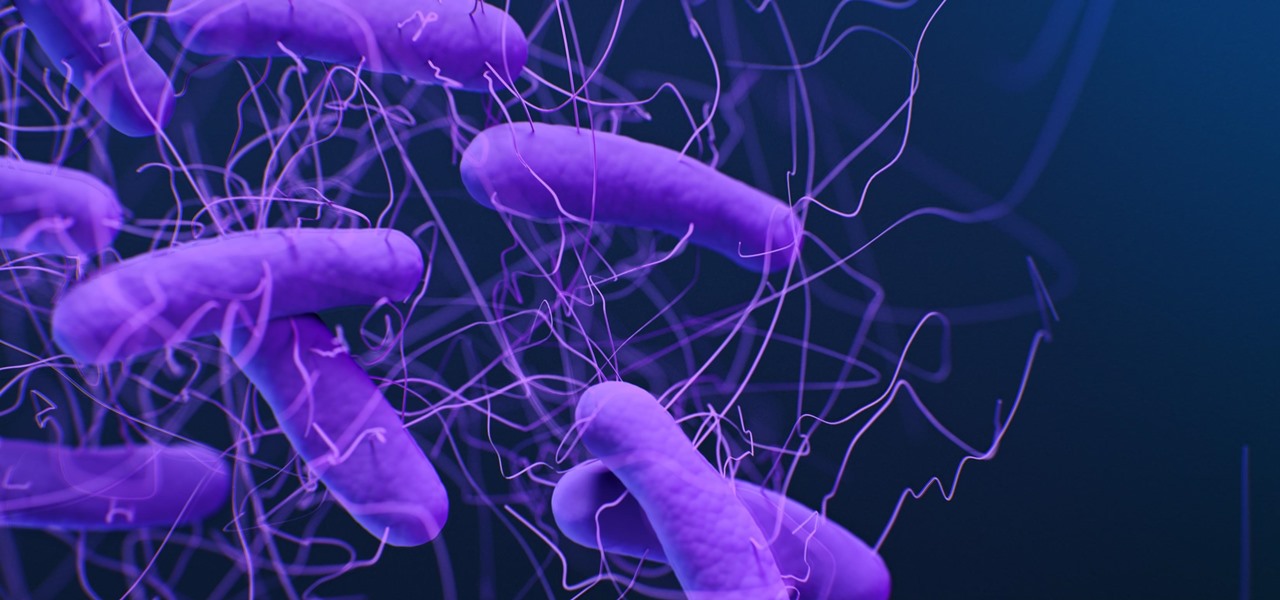
Bacteria from the Clostridia, class are abundant in soil and grow where there is no oxygen. Most of these bacteria produce spores, a dormant phase of the bacteria that can survive acid, heat, radiation, drying, chemicals, and unlike the bacterial itself — even the presence of oxygen — for up to two years.
Clostridium difficile (C. diff) is present in the gut of about 3% of healthy adults and up to 70% of babies and usually doesn't cause disease because the number of Clostridium difficile bacteria is kept very low by the other beneficial bacteria that live in the gut. But when antibiotic use kills good gut bacteria (or someone accidentally ingests spores from contaminated surfaces) fever, gut pain, nausea, and watery diarrhea can signal a C. diff infection. Like botulism, tetanus, and gas gangrene — caused by other Clostridium species — Clostridium difficile symptoms are caused by toxins produced by the bacteria.
Doctors treat C. diff infections with metronidazole, vancomycin, or fidaxomicin. However, about 30% of C. diff infections return and treatment becomes trickier, as the bacteria can become resistant to antibacterials used to treat the infection. Fecal transplants — the process of transferring good gut bacteria by direct injection into the colon — has been shown to successfully treat C. diff infections. About 91% of C. diff infections are cured by fecal transplants, and only about 5.5% of the infections recur.
What we haven't known is how long the good transplanted bacteria live in the recipient's gut. To figure this out, the research team from the University of Alabama at Birmingham had to develop a way to tell the donor and recipient bacteria apart.
Fecal Microbes Transplanted Persist
The research team developed a new method that can detect a single difference in the genetic code of any particular gut bacteria. Using their new technique, the scientists analyzed the genetic make-up of donor bacteria and compared it to bacteria in the gut of fecal transplant patients at different times after their transplant.
They were able to accurately identify transplanted donor microbes in five fecal transplant recipients three to six months after transplant. In two cases, the scientists were able to determine which donor microbes persisted in recipient up to two years after transplantation.
The most common donor microbe identified in fecal transplant recipients were nine species of Bacteroides bacteria, two species each of Alistipes and Parabacteroides, and one species of Acidaminococcus, Akkermansia, Barnesiella, Coprococcus, Eubacterium, Faecalibacterium, Prevotella, and Ruminococcus.
Other research has shown that healthy people have an abundance of Bacteroides in their gut, so persistence of good donor bacteria may be a positive indicator of lasting good health.
The clinical success of fecal microbiota transplantation in treating C. difficile has prompted the consideration of fecal microbiota transplantation to be used for treatment of other gastrointestinal diseases. The results of our analysis provides new insights into the ecology of the human gastrointestinal tract niches that are essential for development of new approaches to improve health via manipulation of this complex microbial community.
Just updated your iPhone? You'll find new emoji, enhanced security, podcast transcripts, Apple Cash virtual numbers, and other useful features. There are even new additions hidden within Safari. Find out what's new and changed on your iPhone with the iOS 17.4 update.





















Be the First to Comment
Share Your Thoughts