Being infected with HIV means a lifetime of antiviral therapy. We can control the infection with those drugs, but we haven't been able to cure people by ridding the body completely of the virus. But thanks to a new study published in Molecular Therapy by scientists at the Lewis Katz School of Medicine (LKSOM) at Temple University and the University of Pittsburgh, all that may change.
The research, led by LKSOM pathologist Wenhui Hu, neuroscientist Kamel Khalili, and radiologist Won-Bin Young, used a new scientific tool called CRISPR/Cas9 to eliminate the virus from mice, even when hidden in the genes of cells.
Why Is This Groundbreaking?
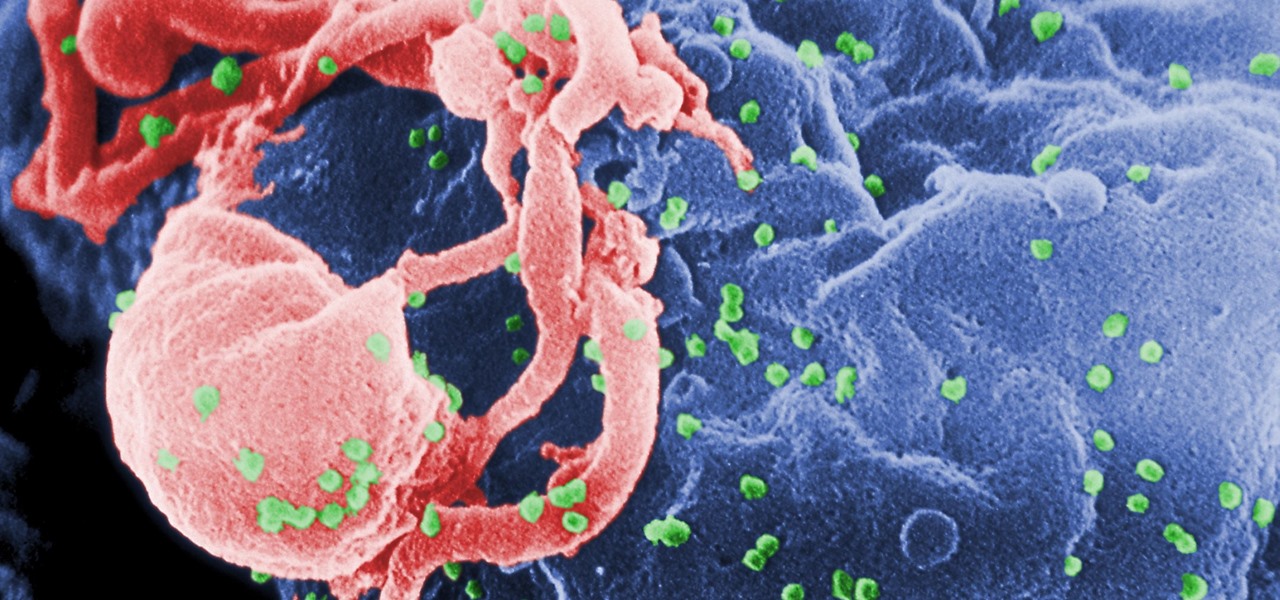
Scientists know that HIV stays in the body — in what's called latent pools — even when it is not detectable by lab tests. The virus hides in immune cells like T lymphocytes and macrophages, and in brain cells, by making a copy of its genetic sequences and inserting them into the cell's genome.
The viral DNA just sits there, waiting. It doesn't replicate — antiviral drugs keep the processes the HIV needs to replicate in check, so the virus can't copy itself. The virus becomes dormant and escapes detection by our immune system since it's hidden away in the genes.
If the patient stops taking their antiviral treatment, the virus can come out of hiding, begin to multiply again, and become detectable by lab tests.
HIV can't be fully "cured" without eliminating the viral genes hiding in these latent pools. One way scientists have theorized we could do this is by using a special viral-DNA cutting system discovered in bacterial cells, called CRISPR/Cas9.
Researchers at Temple University and the University of Pittsburgh put this theory to the test.
Molecular Scissors
The crux of the study by Hu and team was a technique called CRISPR/Cas9. CRISPR is short for Clustered Regularly Interspaced Short Palindromic Repeats — a name that describes the genetic sequence the technique targets. Cas9 is an enzyme that can cut DNA.
In bacteria, these two molecules work as a defensive system, destroying invading viruses by detecting their genetic sequences and cutting the DNA into pieces.
These CRISPR sequences act as a guide, lining up the Cas9 enzymes with a section of DNA it can cut. The sequence that the CRISPR/CAS9 system lines up with is determined by a section of RNA made in the lab, which matches up and homes in on a particular DNA sequence.
The Cas9 enzymes then act like molecular scissors, guided by the RNA molecule. The enzyme cuts the gene, then the cell's natural DNA-repair machinery takes over to mend the gap, which can be repaired in many different ways including deletion of the unwanted gene or replacement with another gene.
Cutting Out HIV Viral DNA
The new research study used the CRISPR/Cas9 technique to cut out the HIV viral DNA that had inserted itself into the of living cells that were the latent pool of infection. They ran three experiments to test out the technique.
The team infected mice with HIV and used the CRISPR/Cas9 system to target and cut the HIV out of the cells. They were able to reduce the detectable virus by 60 to 95 percent. In another experiment, researchers infected mice with a mouse form of HIV, EcoHIV, which multiplies very quickly. After treatment with CRISPR/Cas9, the researchers found no virus in the liver, lungs, brain, or spleen of the mice.
These first experiments showed that CRISPR/Cas9 would cut the HIV DNA and could block the virus from replicating in an active infection.
Next, they tested a model of latent HIV infection. For this experiment, they took mice who had been genetically modified to grow human cells. The mice were implanted with human bone marrow, liver, and thymus harboring chronic HIV infection.
The mice treated with CRISPR/Cas9 had no detectable latent HIV in their human cells.
This research is a huge step forward in eliminating HIV infections for good. Much more work to do before this technique will be ready to test in patients, but once the perfected, scientists are hopeful that it could provide the end to latent HIV — and a cure.
Just updated your iPhone? You'll find new emoji, enhanced security, podcast transcripts, Apple Cash virtual numbers, and other useful features. There are even new additions hidden within Safari. Find out what's new and changed on your iPhone with the iOS 17.4 update.



















Be the First to Comment
Share Your Thoughts