Even though HIV rates declined 18% between 2008 and 2014, 1.1 million people in the US are living with the infection. Part of that is because HIV is treatable, but not curable.
HIV attacks the very cells of the immune system that should kill off the infection, and our bodies don't do a good job of fighting the virus. But, new research from the University of Colorado suggests a way we might be able to get the immune system to develop antibodies to HIV.
There is more than one strain of HIV out there. The more common (and therefore more dangerous) one in the US and worldwide is HIV-1. HIV-2 is less prevalent, less deadly, and is found mostly in western Africa. The two viruses are genetically different enough that they're considered distinct subtypes of the virus.
Some people with HIV produce antibodies to the virus that neutralize it. In most people, this doesn't happen because of a process that protects us from producing antibodies to our cells also happens to prevents the immune system from generating neutralizing antibodies to the HIV-1 virus.
By studying this process, called immune tolerance, the scientists found that HIV-1 virus created a kind of immune camouflage and tested a way to get around it in mice. The research, led by Raul M. Torres at the University of Colorado School of Medicine, was published July 11 in The Journal of Experimental Medicine.
Immune Tolerance of Ourselves
Antibodies are produced by mature B cells of the immune system to antigens — bits of proteins — that we recognize as foreign, like bacteria or transplanted organs from someone else's body. Healthy people don't make antibodies to antigens on their cells — a process called immunological tolerance, which starts in the womb.
The body destroys B cells that might make antibodies to "self" proteins while they are still growing in our bone marrow. If any self-recognizing B cells manage to escape this surveillance and enter the circulation, secondary mechanisms in the immune system prevent them from maturing. These same systems may be stopping the body from creating blocking antibodies to HIV proteins that are similar to the proteins in our bodies.
The neutralizing antibodies produced by some HIV patients are called "broadly neutralizing antibodies" since some of them also recognize some of the body's antigens as foreign. Even in HIV-1-infected people who do make these antibodies, it can take a long time for their efforts to be successful, because their body tries to prevent the formation of any antibodies that could be self-reactive and target healthy tissues.
When self-reactive — also called auto-reactive — antibodies develop to healthy tissue, it can cause autoimmune diseases like rheumatoid arthritis, which attacks joints, or systemic lupus erythematosus, in which auto-antibodies develop to several cellular components, including DNA. Another research team studied a woman with systemic lupus erythematosus also infected with HIV and found she not only produced self-reactive antibodies, but broadly neutralizing antibodies to HIV-1 that controlled her HIV infection without the need for anti-viral therapy.
Researchers from the University of Colorado School of Medicine have discovered how the process that protects the body from autoimmune disease also prevents the immune system from generating antibodies that can neutralize the HIV-1 virus, then found a way around it. They also found the broadly neutralizing antibodies to HIV-1 work by recognizing an HIV viral envelope protein called Env.
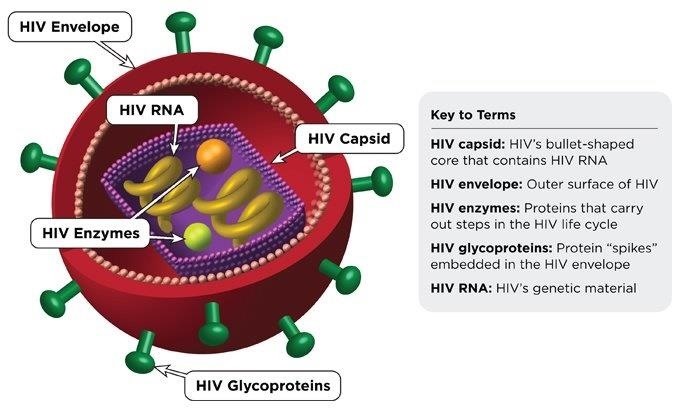
Turning Off the Immune System to Turn It On
The new research found that — in mice — the immune tolerance systems were to blame when B cells couldn't produce HIV-1 antibodies. The researchers studied a mouse experimental model of the autoimmune disease systemic lupus erythematosus, which impairs immune tolerance. When the research team injected the mice with alum, a chemical that is used to increase antibody creation during vaccination, they produced broadly neutralizing antibodies against HIV-1.
When normal, healthy mice were treated with a drug to turn off immune tolerance, they began to make HIV-1 neutralizing antibodies. Alum increased production of the antibodies, and if the researchers also injected the mice with the HIV-1 protein Env, the mice produced strong broadly neutralizing antibodies against a range of different HIV-1 strains.
Mice which produced broadly neutralizing antibodies against HIV-1 also produced auto-antibodies against a chromosomal protein called Histone H2A. Histone H2A antibodies are commonly found in people with lupus, and the researchers confirmed that the anti-H2A antibodies were able to neutralize the HIV.
Torres said that the HIV-1 Env protein may have evolved to be similar to antigens on histone H2A to escape detection by the immune system. It would also explain why antibodies to HIV-1 Env also recognize histone H2A.
While this new information might be used to help scientists develop a vaccine that can stimulate the production of neutralizing antibodies to help cure HIV infections, the study authors said that turning off immune tolerance even transiently must be approached with caution to avoid inadvertently causing detrimental autoimmune diseases.
Just updated your iPhone? You'll find new emoji, enhanced security, podcast transcripts, Apple Cash virtual numbers, and other useful features. There are even new additions hidden within Safari. Find out what's new and changed on your iPhone with the iOS 17.4 update.




















2 Comments
I have questions: Since intial/quick HIV tests (by salivary swabs) test for HIV antibodies to determine if a person is positive, what information is missing from this article? Does the virus then "hide" from the initial antibodies? They're not destroyed since once a patient tests positive, they always do so even on treatment and undetectable. What am I missing, here?
Hi Miguel: To answer your questions: The body creates antibodies against proteins from all different parts of the HIV virion. While the body successfully creates lots of different antibodies (and they can be used in testing to see if the person is infected), they aren't all effective at helping the immune system detect and destroy the virus. Hope that answers your question!
Share Your Thoughts