A new study has found that up to half of people who think they have a penicillin "allergy" can still receive the drug, and other antibiotics with similar structures, without any negative reactions to the meds. Why? Because they're not really allergic, doctors say.
In truly penicillin-allergic people, doctors need to find other drugs to treat their infections, and those drugs are often less effective and more toxic. And antibiotics that don't completely kill bacteria can encourage antibiotic-resistance—because the bacteria that survive are the ones not sensitive to the drug, and those multiply and spread.
If some people who thought they were allergic to penicillin really weren't, we might be able to use an old drug to treat the new class of bacteria that most other antibiotics don't work on anymore.
That's the idea behind research conducted by Massachusetts General Hospital and Brigham and Women's Hospital in Boston, which was published online in the Journal of Allergy and Clinical Immunology last month.
"From 10 to 15% of hospitalized patients have penicillin allergy in their medical record, but studies have shown that more than 95% are not really allergic," said study researcher Dr. Kimberly Blumenthal in a press release from Mass General Hospital.
Not All Penicillin Allergies Are Created Equal
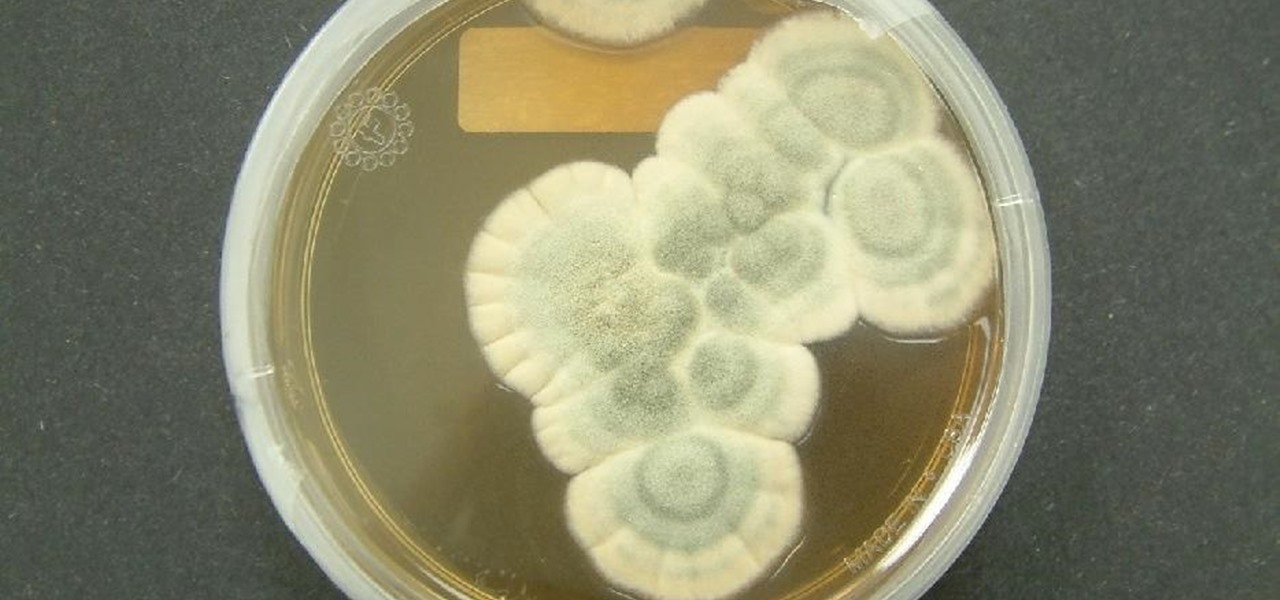
When Alexander Fleming discovered the antibiotic properties of a common mold in 1928, we thought we had the magic bullet to kill infections in their tracks—and we did. It cured untold millions of infections. Now, just a few years short of a century later, a significant number of people are allergic to the drug, and many more have infections which have become resistant to it.
Natural and semi-synthetic penicillins have been developed, most notably penicillin V and amoxicillin, but both also can cause allergic reactions if someone is sensitive to penicillin itself.
There are two different types of allergic reactions to penicillin. An acute allergic reaction happens rapidly within minutes to a couple hours after treatment when the patient develops sudden anaphylaxis—an extreme and life-threatening allergic reaction—with low blood pressure, difficulty breathing, swelling, hives, and eventual collapse of the cardiovascular system.
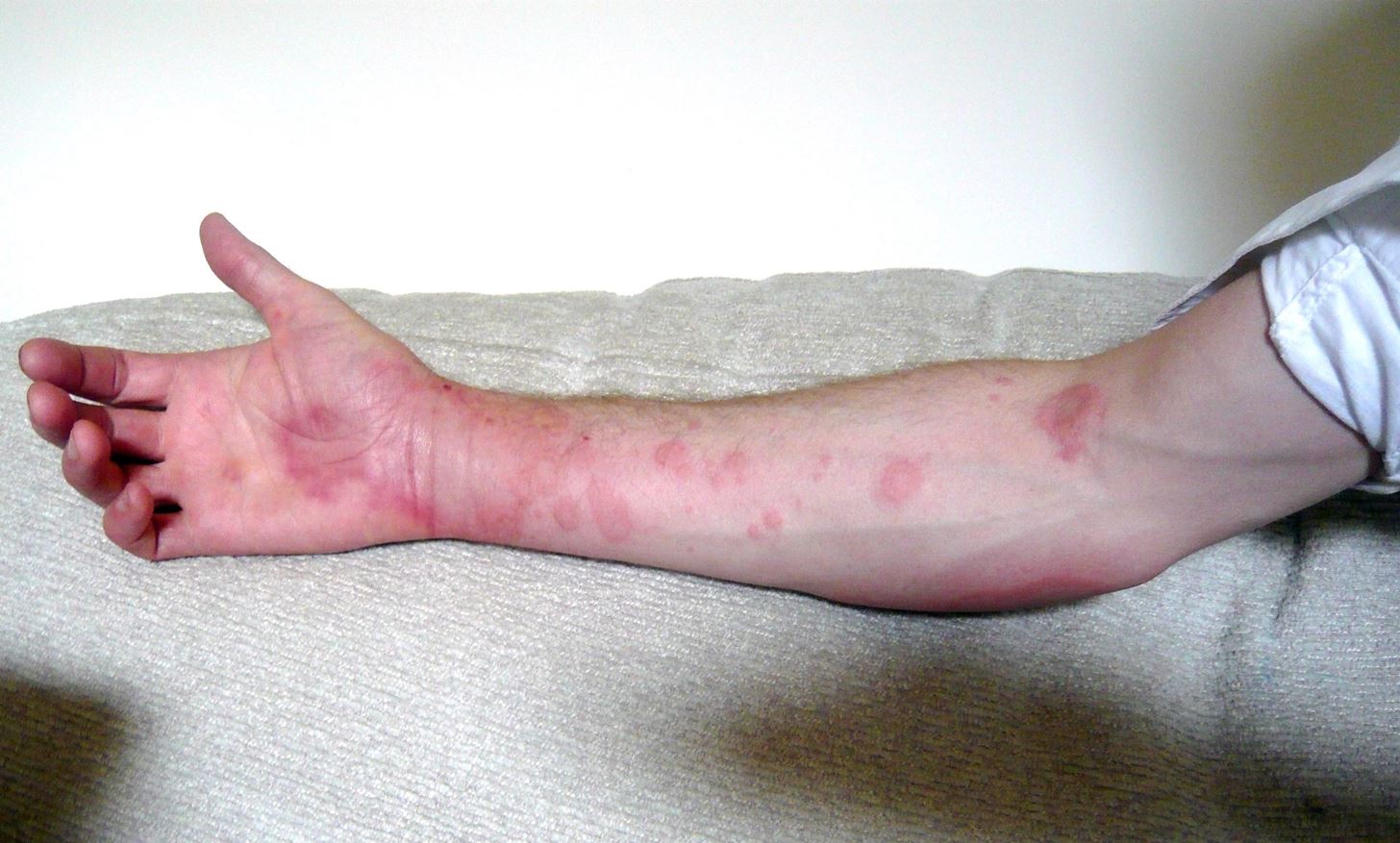
Acute reactions usually occur after the body reacts to a previous penicillin treatment by forming IgE antibodies, the antibodies formed as part of allergic responses. In a subsequent exposure, the penicillin binds to the IgE and signals mast cells to release histamine, the culprit and cause of anaphylaxis. This makes the second reaction (if the patient is given penicillin again) much quicker and more dangerous.
A less serious allergic reaction can occur 7–10 days after a subsequent penicillin treatment. This reaction occurs if IgG antibodies were formed in response to the first penicillin treatment. In this case, the IgG reaction results in inflammation, hives, fever, and joint pain.
Unfortunately, most people aren't aware if they formed IgE or IgG antibodies to their previous treatment with penicillin. Alternatively, other negative reactions, including those related to their actual infections, can be misread by patients as an allergic reaction, as well.
Getting the Right Treatment
By using tools like skin testing (to see if penicillin caused a skin reaction), or use of a computerized treatment guideline and decision support system questionnaire to figure out of the person actually did have an allergic reaction, the study investigators were able to determine that many of these reactions don't necessarily leave a lasting allergy.
The researchers analyzed the results of inpatients who had a recorded penicillin allergy, but needed antibiotic treatment. Over a two year period, the patients either received the usual care with non-penicillin antibiotics, the skin testing, or the questionnaire.
- Skin tests were performed by applying injections of different penicillin concentrations under the skin. If they had no reaction, the patient was determined not to be allergic. Patients with negative skin tests were given an oral dose of amoxicillin, a semi-synthetic form of penicillin.
- The computerized system used a series of questions about the patient's past allergic reactions to penicillin, such as whether the patient experienced a rash, fever, or joint pain. The severity of the reaction was used to decide whether the patient could receive penicillin or cephalosporin—an antibiotic an allergic patient might react similarly to.
- Use of the penicillin skin testing and the computerized questionnaire both increased use of penicillin and cephalosporin antibiotics among the people with reported penicillin allergies.
Patients who underwent skin testing were six times more likely to be given penicillin or cephalosporin, instead of the alternative antibiotics typically used for allergic patients. When the computerized decision guidelines were used, twice as many patients received penicillin or cephalosporin.
While not in widespread use yet, the computerized system easily identified people who thought they were allergic, but weren't. These people could safely be given penicillin for their infections and is an easy-to-implement system.
That means fewer side effects for the patients, and less use of second-line antibiotics that could cause resistance to develop.
Just updated your iPhone? You'll find new emoji, enhanced security, podcast transcripts, Apple Cash virtual numbers, and other useful features. There are even new additions hidden within Safari. Find out what's new and changed on your iPhone with the iOS 17.4 update.





















Be the First to Comment
Share Your Thoughts