There are all kinds of theories—many supported by science—about what causes Alzheimer's disease. Tangles of protein called ß-amyloid (pronounced beta amyloid) plaques are prominently on the list of possible causes or, at least, contributors. An emerging theory of the disease suggests that those plaques aren't the problem, but are actually our brains' defenders. They show up to help fight an infection, and decades later, they become the problem.
That theory, along with some provocative evidence supporting it, has been published in several journals by Dr. Robert Moir, a researcher at the MassGeneral Institute for Neurodegenerative Disease, and Assistant Professor in Neurology at Massachusetts General Hospital and Harvard Medical School.
Sometimes associated with the loss of cognitive function that accompanies old age, Alzheimer's disease is a distinct type of memory loss characterized by progressive dementia. Symptoms such as memory loss usually progress slowly as the disease advances through the brain. Eventually, patients become increasingly disoriented; confused about events, time, and places; and suspicious. In later stages, they experience difficulty speaking, swallowing, and walking.
Usually, a definitive diagnosis of Alzheimer's disease is made after the patient dies and an autopsy can be performed. The presence of ß-amyloid plaques in the brain are diagnostic of Alzheimer's.
The current popular theory to explain the development of Alzheimer's disease is called the amyloid cascade hypothesis. ß-amyloid plaques accumulate in the brain from ß-amyloid peptides, which are short pieces of protein. This accumulation drives a cascade that involves generation of neurofibrillary tangles from a protein called tau. These changes lead to loss of connectivity between brain neurons, their eventual death, and progressive dementia.
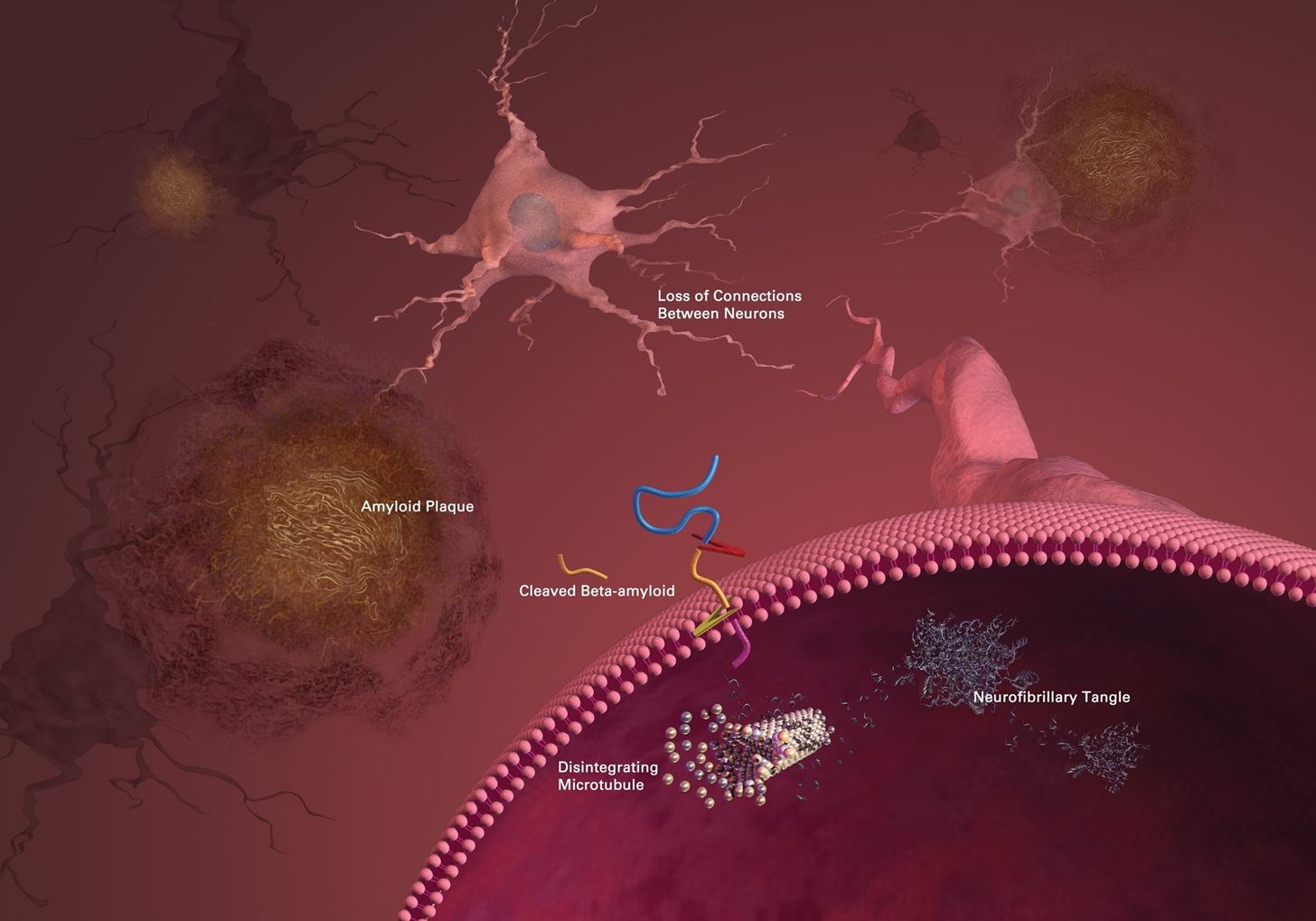
Moir does not dispute that ß-amyloid is a player in the development of Alzheimer's disease, but he has formed the pathogen hypothesis—a theory in which ß-amyloid plaques play a defensive role in the brain, but eventually, their accumulation goes out of control, resulting in neuronal damage and dementia.
In Moir's theory, the formation of the plaques is not the seminal event in Alzheimer's disease—an infection is. Several different types of infection have been implicated in this process and it isn't clear, proven, or even implied that the infection causes Alzheimer's. In Moir's theory, the ß-amyloid peptide arrives to help after an infection takes hold, then starts the cascade that ends decades later in Alzheimer's disease.
The findings of Moir and his colleagues have met with strong opposition—and strong interest. The scientific evidence on each side is strong, too.
Bucking Dogma
In support of his hypothesis, Moir conducted several studies aimed at elucidating the role of ß-amyloid in Alzheimer's disease.
In a 2010 PLoS One publication, Moir and his team of researchers showed that ß-amyloid was able to kill or weaken eight common microorganisms. When the researchers added in antibodies to ß-amyloid to stop it from working, the antimicrobial activity stopped, implicating ß-amyloid as the microbe killer.
The potency of ß-amyloid's antimicrobial activity was similar or greater to that of antimicrobial peptide LL-37. The comparison to LL-37 is both interesting and relevant.
LL-37 is also a peptide—a piece of protein—and it has been shown to possess antimicrobial activity against microorganisms. It is expressed in epithelial cells of the testis, skin, the gastrointestinal tract, and the respiratory tract, and in immune cells. It is active in the body's response to infections, inflammation, and wound healing.
Just as the LL-37 peptide is part of the body's natural defense, it could make sense that ß-amyloid is acting in the same way, but for the brain. ß-amyloid is a peptide, and Moir's findings suggest it is also antimicrobial and produced in the body, for the body.
In the May 2016 issue of Science and Translational Medicine, Moir and colleagues presented their findings on studies in test tubes, mouse, and worm models of Alzheimer's disease. Of course, Alzheimer's can't be given to humans just because we want to study how it develops—and we can't do that anyway because we don't know what causes it. Mice are a good model because they can be genetically modified to lack the ß-amyloid, so deposits can't accumulate, tau protein tangles don't form, and these mice don't get Alzheimer's. These Alzheimer's resistant mice make a nice control for experiments.
When normal mice brains are injected with Salmonella, they accumulate amyloid plaques within hours, and the plaques helped them to live longer than the infected mice without ß-amyloid, which didn't develop plaques. Amyloid's benefit, however, ran out when the pathogen died, the plaque remained, and the cascade took over.
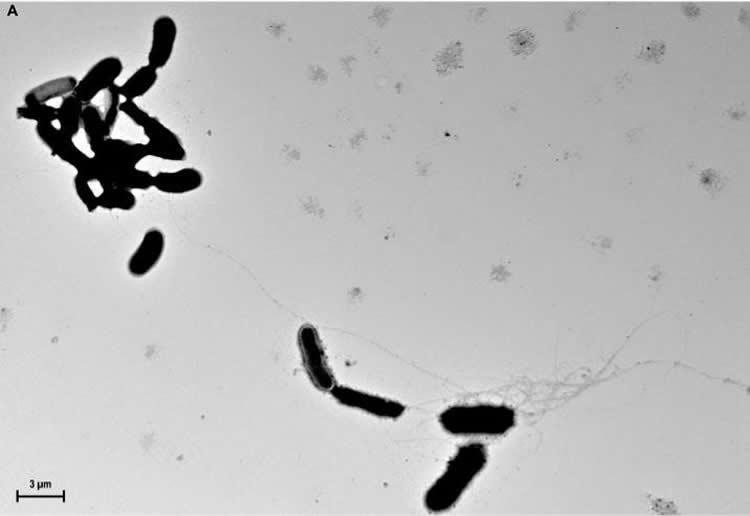
ß-amyloid peptides in petri dishes attached themselves to a yeast called Candida albicans, then they create fibers that wrapped around and trapped the microbes in a protective bundle. When this same experiment was done in worms, the protective bundles prevented C. albicans from infecting the worm.
These new experiments showed that, in experimental models, a brain infection with Salmonella caused ß-amyloid to accumulate and ß-amyloid peptides were capable of trapping microbes and preventing infection.
Keep Your Friends Close...
A fair amount of historical observations lend support to Moir's hypothesis, but there is a gap in the connection between active, diagnosed brain infections and Alzheimer's disease. Like the diagnosis of Alzheimer's, most brain infections are diagnosed on autopsy, if they're tested for at all.
The brain is a special part of the body because it's not linked up to our vascular system and full of blood like the rest of our tissues. The blood-brain barrier helps to restrict the passage of protein and cells, including pathogens, from the blood to the brain. It is composed of endothelial cells that line vessels in the brain. Unfortunately, some bacteria in the blood can infiltrate the junctions between the endothelial cells and penetrate the blood-brain barrier. This is how bacteria like Neisseria meningitidis, Streptococcus pneumoniae, and Haemophilus influenzae cause meningitis.
Several types of brain pathogens have been found in brain autopsy material from Alzheimer's patients.
As early as 1986, in a letter to the editor of the Journal of the American Medical Association from pathologist Alan MacDonald described Borrelia seen in the brains of patients who died of dementia. Later, he isolated Borrelia burgdorferi, the spirochete that causes Lyme disease, from autopsy brain tissue from a patient with Alzheimer's disease.
In 1998, Brian Balin, now director of the Center for Chronic Disorders of Aging at the Philadelphia College of Osteopathic Medicine, and his colleagues found Chlamydia pneumonia DNA in the brains of 17 of 19 Alzheimer's brains, but in only 1 of 19 non-Alzheimer brains, providing indirect evidence that Chlamydia infection was associated with Alzheimer's.
Priya Maheshwari and Guy Eslick from the University of Sydney, in Australia, performed a meta-analysis of 25 studies investigating the association of infections with Alzheimer's disease. Their results were published in 2015 in the Journal of Alzheimer's Disease. They found a ten-fold increased occurrence of Alzheimer's disease when there was evidence of infection with spirochetes, and over a five-fold increase when evidence of C. pneumonia was present, compared to the occurrence of Alzheimer's when no infection was present.
These observations only showed an association of pathogens, via their presence, in the brain of people with Alzheimer's. But still, there was no evidence specifically linking these agents to causing the disease.
Clearly, scientific evidence exists to support a role for pathogens in the development of Alzheimer's, and Moir has worked to define that role. Still, many gaps in the relationship of infection, ß-amyloid, and Alzheimer's Disease remain, and the exact cause of Alzheimer's disease has not been identified.
Will the pathogen hypothesis come to the fore and become a mainstream line of investigation for Alzheimer's or will Moir be shamed for his hypothesis like Barry Marshall, who eventually drank a concoction containing Helicobacter pylori to prove the bacteria caused the infection?
It seems that the tides are turning in Moir's direction. Journalist Melinda Wenner Moyer talked to him for a story at Aeon in which he recounted a recent event:
At a neurodegeneration conference held in Korea in 2016, Moir says attendees were asked to raise their hands if they thought infections might be involved in Alzheimer's, and a majority of hands went up. 'Ten years ago, it would have been four guys in a corner, all huddled together, not talking to anyone else,' Moir says. 'My impression is that this is an idea whose time has come.'
In March 2016, 33 international researchers from 12 countries cosigned an editorial in the Journal of Alzheimer's Disease . They implored others to consider that Alzheimer's disease could have an infectious cause and sent out a major call to action to the scientific world—that they pursue research into the link between infection and Alzheimer's disease. Further, they argued that, based on scientific evidence like Moir's, clinical trials of antimicrobial agents to treat Alzheimer's disease are now warranted. Their editorial cited 79 references, the majority of which reported on studies into infectious causes of Alzheimer's disease.
Obviously, the pathogen hypothesis is gaining momentum. Maybe, just maybe, the future will present a new direction down the tangled path to development of Alzheimer's disease.
Just updated your iPhone? You'll find new emoji, enhanced security, podcast transcripts, Apple Cash virtual numbers, and other useful features. There are even new additions hidden within Safari. Find out what's new and changed on your iPhone with the iOS 17.4 update.





















Be the First to Comment
Share Your Thoughts