Most of us equate feeling cold with catching a virus—but we've also heard plenty of debunkers proselytizing that being cold isn't what gives you the flu.
Still, we know that cold and flu season always falls during the winter, so exactly what is the relationship between winter and the flu or colds? Are they passed along more just because we're inside all the time or, as some new research suggests, does the cold and dry air help the viruses along?
"According to our calculations, a cold week with an average temperature below 0° Celsius [33° Fahrenheit] precedes the start of the flu epidemic," Swedish researcher Nicklas Sundell, an infectious diseases specialist at the University of Gothenburg, said in a recent press release.
Sundell and his colleagues published the results of their research into the relationship between outdoor climate and viral respiratory tract infections in the Journal of Clinical Virology.
Baby It's Cold Outside—& Some Viruses Love It!
The research team measured respiratory pathogens in over 20,000 clinical nose and throat swab samples collected between October 2010 and July 2013 at the Sahlgrenska University Hospital in Gothenburg, Sweden. They compared the viruses they found in the samples with outdoor temperature and humidity recorded at the same date and time as the sample collection and analyzed the results over time.
A decrease in temperature was followed the next week by a significant spike in the number of swabs containing influenza A virus. The data revealed that a quick drop in temperatures to below freezing preceded the start of the annual flu epidemic in each year they studied.
The authors suggested that a drop in temperature and vapor pressure during cold outdoor weather may extend the length of time when infectious influenza droplets remain airborne, increasing the chance of infecting new hosts, setting up conditions for an outbreak or epidemic.
A drop in temperature or humidity did not seem to affect the infection rates of two common cold viruses, the rhinovirus or enterovirus. The researchers concluded that these viruses probably spread through routes of infection other than aerosols.
Sundell and his co-authors did not speculate on the route, but viruses can be transmitted by contact with contaminated objects, fluids, or infected people, so these may be the preferred routes of transmission of the common cold.
The Flu Season So Far This Year
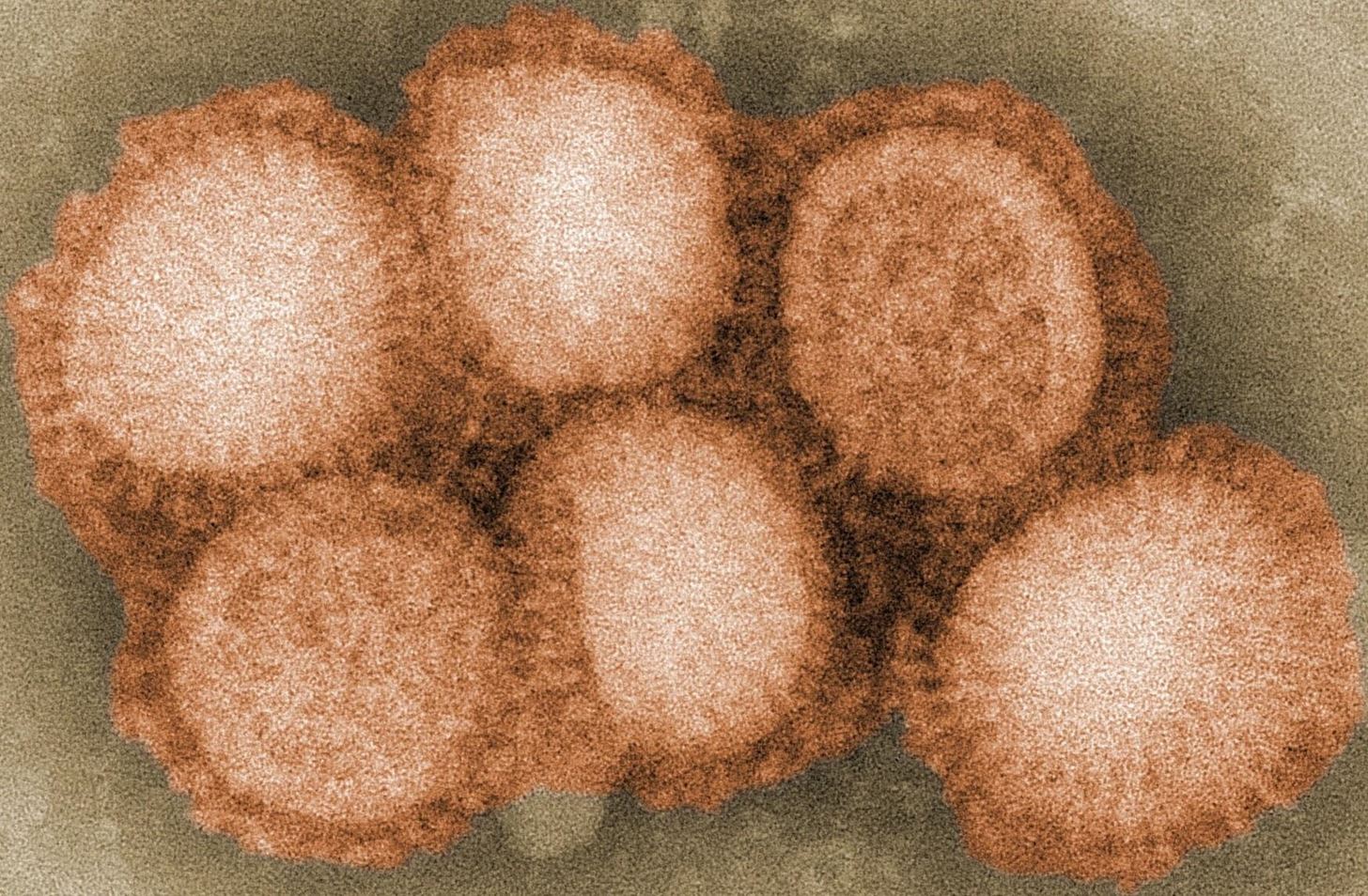
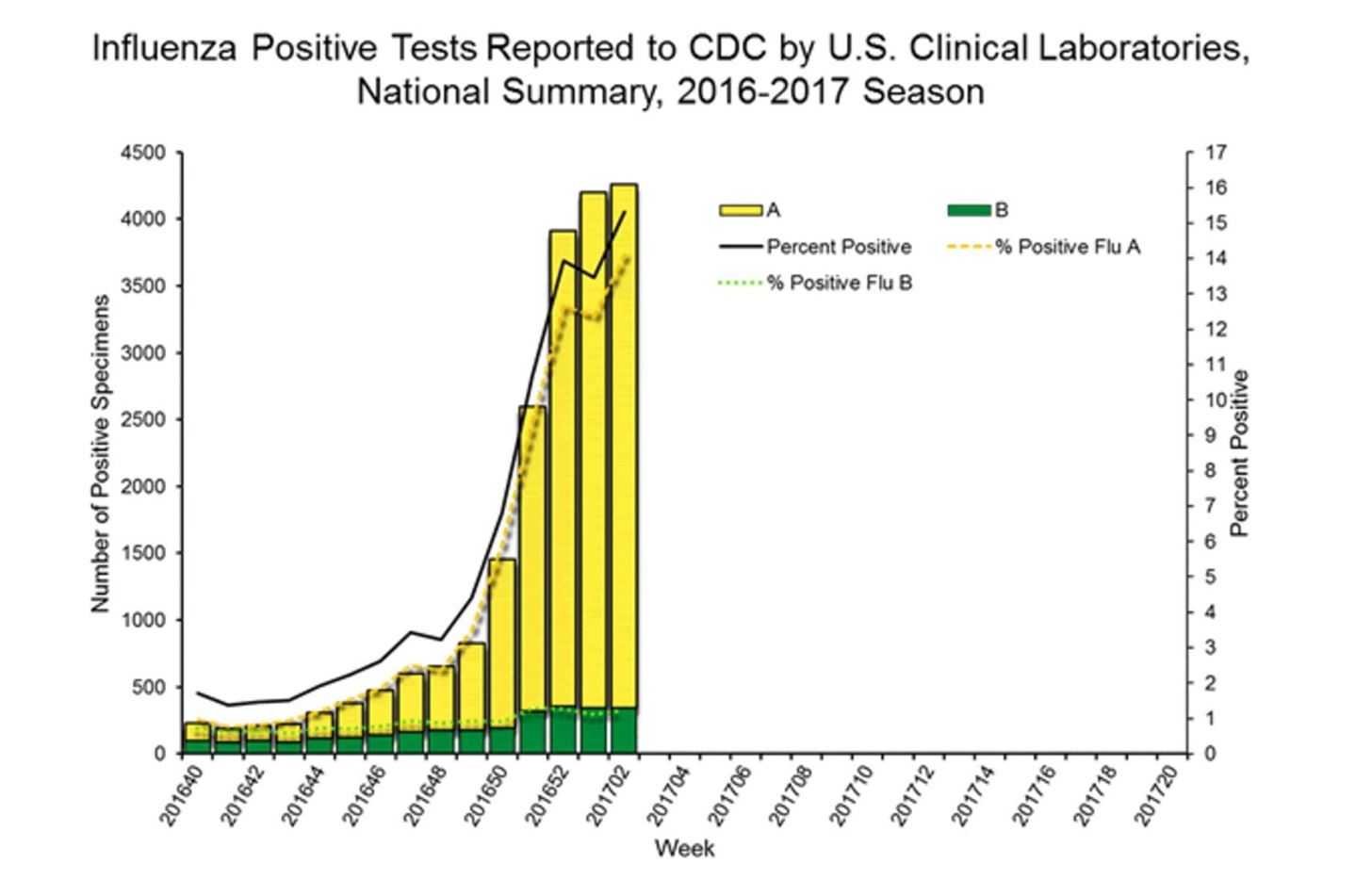
Reports from the Centers for Disease Control and Prevention (CDC) for the second week of 2017 show 4,258 confirmed cases of the flu. Most of the cases—92%—are a type of influenza A virus. It looks like the cases are still rising weekly, so we probably haven't hit the peak of flu season yet.
The flu vaccine being used in the 2016-2017 season includes protection against influenza type A (H1N1- and H3N3-like viruses) and type B (B/Victoria lineage) viruses, as well as another type B strain (B/Yamagata lineage) in some instances.
The flu vaccine cuts your risk of getting the flu approximately in half and can cut the risk even more in people with chronic illness, the very young, and the very old.
The risk of getting the flu is somewhere around 10-20%, depending on your age and health. That means that 1 in every 5 to 10 people will get the flu unless they are vaccinated against it.
So, especially in the days and weeks of the first real cold snap, try to avoid sick people and crowded places. You can also take the study authors' advice and keep your home and work space well humidified to help discourage transmission of the flu virus at least in the direct spaces around you. Any old humidifier should be able to cut down the dryness in your work area.
When you're out and about, the dry flu in the air may be a bit harder to avoid. Cover your mouth and nose and be sure to keep your hands washed—and get your flu shot!
Just updated your iPhone? You'll find new emoji, enhanced security, podcast transcripts, Apple Cash virtual numbers, and other useful features. There are even new additions hidden within Safari. Find out what's new and changed on your iPhone with the iOS 17.4 update.






















Be the First to Comment
Share Your Thoughts