Type 1 diabetes is an attack on the body by the immune system — the body produces antibodies that attack insulin-secreting cells in the pancreas. Doctors often diagnose this type of diabetes in childhood and early adulthood. The trigger that causes the body to attack itself has been elusive; but many research studies have suggested viruses could be the root. The latest links that viruses that live in our intestines may yield clues as to which children might develop type 1 diabetes.
An international team of researchers from the US, Finland, and Estonia studied the viruses in the intestines of children at high-risk of developing type 1 diabetes from birth until some developed antibodies associated with type 1 diabetes. They compared the gut viruses of these children to those from similar children who did not develop diabetes. The children whose bodies created antibodies against the pancreas had fewer different types of viruses in their gut, with one type particularly reduced.
Lead authors Guoyan Zhao and Herbert W. Virgin, from Washington University School of Medicine in St. Louis, MO, published the new research on July 10 in the Online Early Edition of PNAS.
Type 1 Diabetes
There are about 1.25 million people in the US with type 1 diabetes, with another 40,000 or so diagnosed each year. In type 1 diabetes, antibodies to the pancreas prevent the body from making insulin. Because the antibodies are to parts of our own body, they are called auto-antibodies. can detect auto-antibodies in the blood of infants as early as one year of age or sooner, but symptoms of the disease may not appear until late childhood or early adulthood.
Since we need insulin to absorb sugars into our cells from the bloodstream, sugar (glucose) accumulates in the blood of people with type 1 diabetes. Symptoms of diabetes are increased thirst, urination, and hunger; feeling fatigued; experiencing blurred vision; weight loss; numbness in hands or feet; and sores that don't heal. Lab tests can distinguish type 1 diabetes from type 2 diabetes, a disorder where the body doesn't use insulin properly. People with type 1 diabetes must measure their blood glucose throughout the day, take insulin by injection or use an insulin pump, and monitor the types and amounts of food they consume to achieve acceptable blood glucose levels.
So far, the disease is not preventable, and no one knows what causes type 1 diabetes. It has been associated with certain genes, like Human Leukocyte Antigen (HLA) genes HLA-DRB1, -DQA1, and -DQB1; an insulin gene on chromosome 11p15; and genes that code for components of the immune system. Development of type 1 diabetes has also been associated with particular viral infections, including coxsackie B virus, German measles, mumps, and rotavirus — a diarrhea-causing infection. The scientists' theory for how viruses might cause diabetes starts when the virus enters the body. The immune system starts to produce antibodies to fight the infection. If cells of the immune system see some of the same proteins on the insulin-making cells of the pancreas as on the invading virus, the immune system may turn on the pancreas to kill those cells as well.
But, not everyone who has those genes or has had those infections develops the disease and researchers continue to search for what triggers the disease in certain people. One place they have been looking is in our gut.
The Intestinal Virome
The gut microbiome — the community of microorganisms that live in our intestines — is made up of bacteria, archaea, viruses, and fungi. Our intestinal virome is the subset of viruses that are contained within our microbiome and includes both eukaryotic viruses — viruses that infect the cells of organisms like animals and plants — and bacteriophage, which infect bacteria.
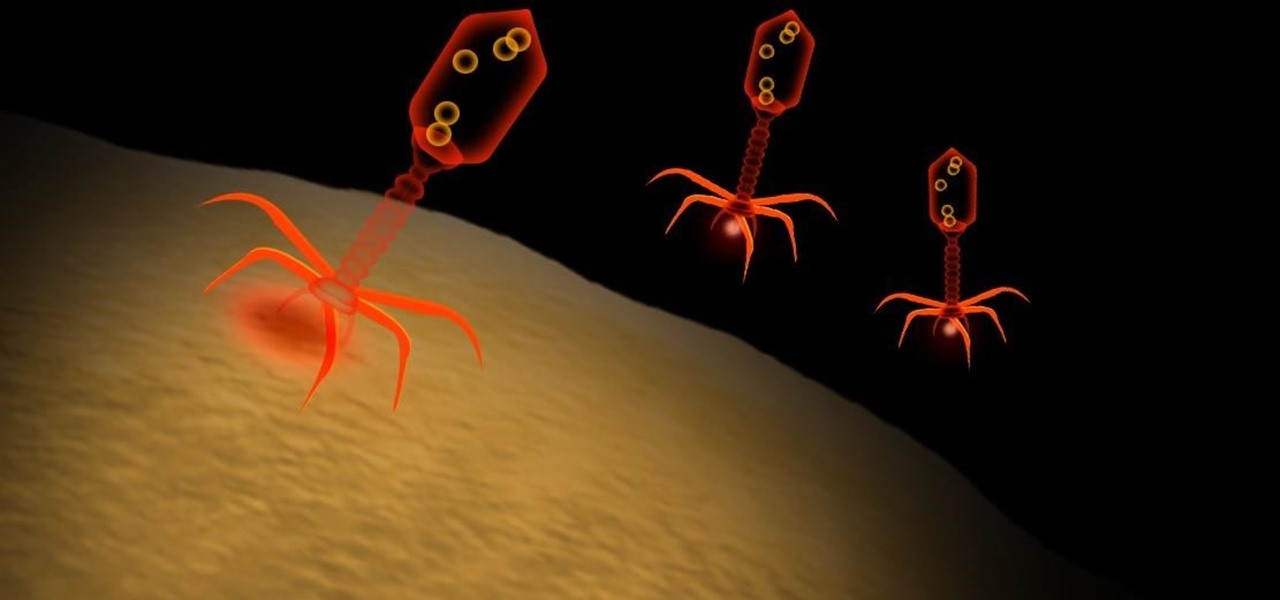
Bacteriophage are the most abundant viruses in our healthy gut. They consist of a core of genetic material (RNA or DNA) surrounded by a protein capsule. Bacteriophage exist as one of three structures: As a 20-sided head with a tail, a 20-sided head without a tail, or in filamentous form. They all infect bacteria, causing them to break apart, and play a role in keeping the numbers of disease-causing bacteria down and maintaining populations of healthy bacteria. It's been estimated that anywhere between 35 to 2800 viruses live in the gut of a healthy person.
A previous research study sought to determine the bacteriophage present in the gut of healthy people by analyzing stool samples. They found viruses from the Caudovirales order: Podoviridae, Siphoviridae, and Myoviridae. Bacteriophage have narrow host ranges — different phages infect only certain bacteria. For example, one type of Poloviridae bacteriophage infects Clostridium difficile, the bacteria causing a severe gastrointestinal infection.
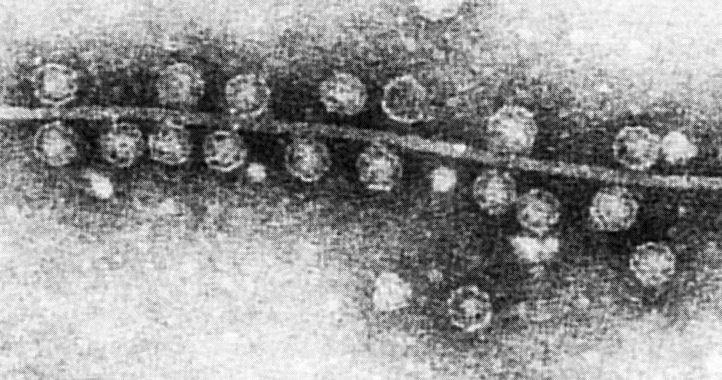
While the virome of a healthy individual is believed to be stable over their lifetime, only a few studies have been done comparing the virome composition between people or evaluating its change with disease development.
The objective of the new research study was to evaluate the virome in children at risk for type 1 diabetes to potentially identify viruses associated with either disease risk or protection from the disease.
Intestinal Virome and Type 1 Diabetes
The research study by Zhao, Virgin, and their team, examined RNA and DNA intestinal viruses from 220 fecal samples taken from 11 children at risk for type 1 diabetes because of their HLA gene type; all of whom developed antibodies against their pancreatic cells. Parents collected these samples monthly, from birth through a time when antibodies to islet cells — the insulin producers — developed, most often between the ages of one and three. Fecal samples taken during the same period from 11 children who did not develop antibodies were controls for comparison.
There was more intestinal virome diversity in the samples from control children than in the children who developed type 1 diabetes auto-antibodies. However, the researchers didn't find a correlation between eukaryotic viruses previously linked to type 1 diabetes.
There was a greater abundance of genetic sequences associated with the eukaryotic virus Circoviridae in control subjects compared to the children with auto-antibodies. The study authors felt the presence of these eukaryotic viruses might be protective against the development of type 1 diabetes and need to be studied in a greater number of children.
Children in the control group had more different kinds of bacteriophage in their gut than in the children who developed antibodies against islet cells. The researchers found pecific sequences associated with bacteriophage that infect a bacterial resident of healthy guts, Bacteroides in the children who developed auto-antibodies. The study authors speculated that the bacteriophage present in the children with antibodies could alter the bacterial microbiome in the course of developing type 1 diabetes.
"Taken together, these findings in a single cohort suggest a model in which the risk for human autoimmunity (in this case type 1 diabetes) is related to a combination of protective vs. disease risk-conferring effects of the virome," the study authors write.
It may turn out that it's not a particular viral infection that triggers type 1 diabetes, but the direction in which the virome balance of eukaryotic viruses and bacteriophage in our gut tip the scales.
Just updated your iPhone? You'll find new emoji, enhanced security, podcast transcripts, Apple Cash virtual numbers, and other useful features. There are even new additions hidden within Safari. Find out what's new and changed on your iPhone with the iOS 17.4 update.






















Be the First to Comment
Share Your Thoughts