Humanity is standing on an infection precipice. As antibacterial resistant grows, we're running out of options, and a recent scary case of total antibiotic resistance is a frighting view of our potential future. In the end, it was septic shock that took the life of a 70-year old woman with an incurable infection. One of few such cases in the US, her death could nonetheless be the shape of things to come.
You may have read the headlines, which looked something like this: "Nevada Woman Killed by Superbug Resistant to 26 Antibiotics." The eye-catching news hit the wires after the release of the Morbidity and Mortality Weekly Report on January 13 from the Centers for Disease Control and Prevention.
Millions of people catch treatment-resistant bacteria every year, but this case is unique. It's rare enough that it could be the first of its kind, and we knew about the bacteria's resistance long before it happened.
While antibiotic-resistant bacteria currently sicken about 2 million people and kill about 25,000 of those every year in the US, completely resistant cases like these could become the norm—propelling that number exponentially higher. Many infections like this usually still respond to one or two "last line" of defense antibiotics.
The recent Morbidity and Mortality Weekly Report outlines the case with its own headline that, for those of us outside the medical profession, might not raise a lot of interest:
Notes from the Field: Pan-Resistant New Delhi Metallo-Beta-Lactamase-Producing Klebsiella pneumoniae — Washoe County, Nevada, 2016
Flowing from that headline is a five-paragraph summary of a battle, which was, in the end, between one woman and the untreatable bacteria that overran her body. For her, there were no options. All lines of defense were breached. There was nothing left to try.
"Before, we could go to carbapenems, and they could reliably squash the bugs," Dr. James Johnson, Professor of Medicine and Senior Associate Director of the Infectious Diseases Fellowship Program at the University of Minnesota, told NPR. "This case broke down even our last great gun."
The facts of the case are somewhat straightforward. After an extended trip to India, a woman who resided in Washoe County, Nevada, returned home in early August of 2016. Within two days she was admitted to an acute care facility diagnosed with systemic inflammatory response syndrome, better known as SIRS.
More than 20 years ago, criteria for SIRS were created to catalog and diagnose the sometimes dangerous response of the human immune system to severe infection. SIRS criteria help pinpoint how far along a patient is toward full-blown septic shock, and also establish criteria for entry into clinical treatment trials.
The patient had broken her right femur, the long bone connecting hip and knee, approximately two years prior to her final hospital admittance. While in India, the patient was hospitalized several times for a serious bone infection called osteomyelitis, and accumulation of fluid near her hip, associated with her earlier femur fracture. Before returning to the States, she had been hospitalized as recently as June 2016.
Carbapenem-resistant Enterobacteriaceae (CRE) is a highly drug-resistant family of bacteria that include species like Klebsiella pneumoniae and Escherichia coli. Infections with these bacteria produce New Delhi metallo-beta-lactamase (NDM), an enzyme that protects the bacteria from antibiotic drugs.
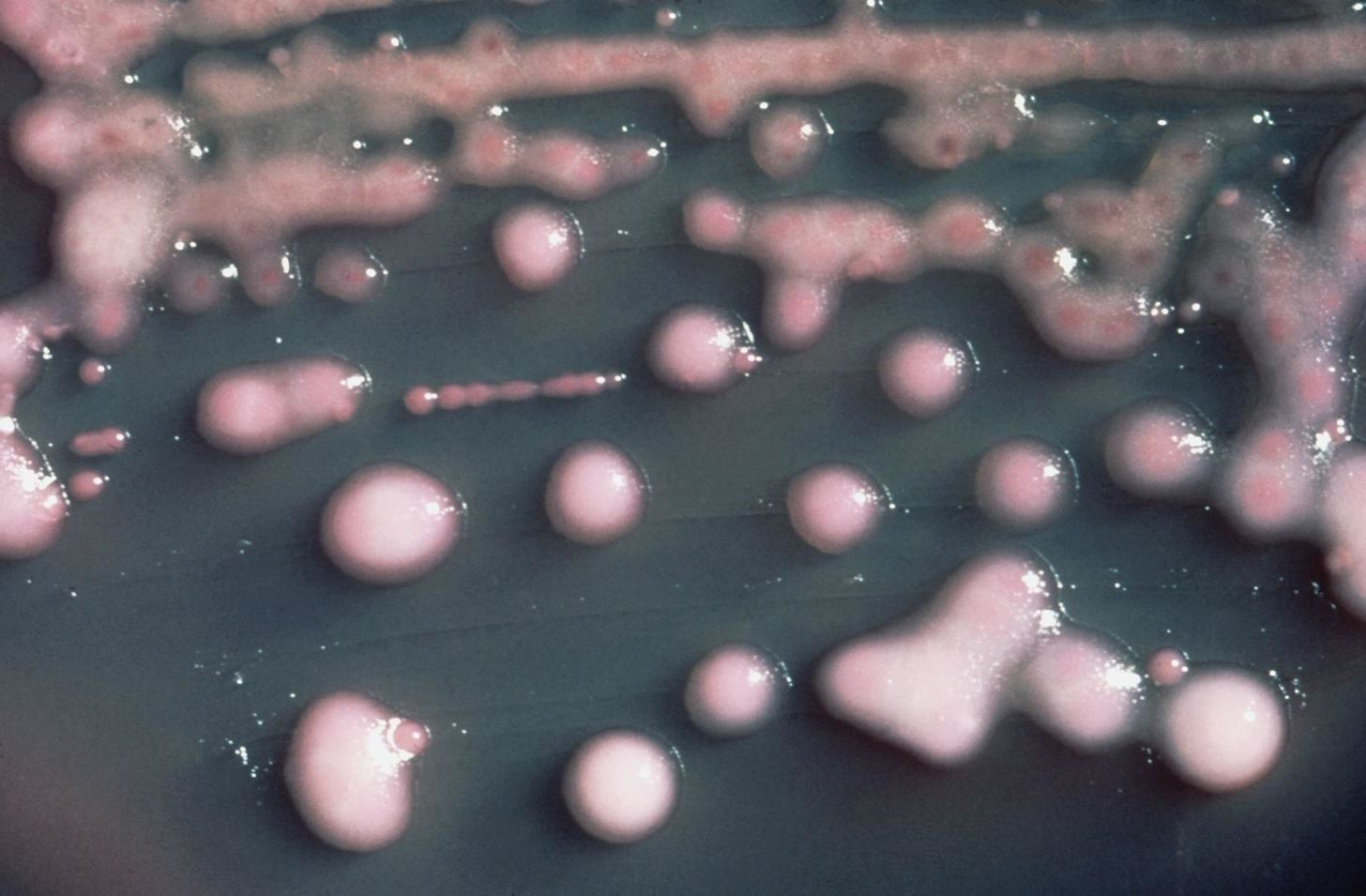
Once her infection was identified, the patient was isolated in a room by herself with precautions in place to prevent spread of the infection. Testing revealed her infection was resistant to all 26 antibiotics that could have potentially been used to treat her.
In early September, with no effective treatment possible, the patient went into septic shock, a condition whereby the immune system mounts a virulent inflammatory attack on invading pathogens that causes a dramatic drop in blood pressure and rapid organ failure. The woman died. No additional infections were identified in the hospital.
"We're off the cliff. It's already happening. People are dying. It's right here, right now," Johnson told NPR. "Sure, it's going to get worse. But we're already there."
Researchers urgently explore new paths to create tools by which we might survive the loss of the drugs, and the rise of the superbugs. On a personal level, consider these simple tips to keep yourself, and loved ones, as healthy as possible:
- Across the board, the leading advice for avoiding infection is to wash your hands well. Sure, you have heard it a lot. Now do it for 20 seconds, front and backs of hands, under nails, and between fingers. Sing along to the "Happy Birthday" or "ABC" song for a little 20-second timer. At home, don't waste your money, or the healthy microbes on your hands, by using antibacterial soap—the US Food and Drug Administration says the science does not support its use.
- Take precautions while handling and cooking food to deter and prevent food-borne illnesses.
- Stay current on vaccines and flu shots. Vaccines protect you, your family, and your community, plus lessen the chances of associated infection.
- Ask healthcare providers to wash their hands, and go ahead and ask to ensure medical equipment is properly sterilized and needles are not reused.
- If prescribed an antibiotic, be sure to talk to your doctor about medical necessity. Antibiotics do not work against viruses, and broad-spectrum antibiotics damage the beneficial bacteria in your body. If prescribed antibiotics, take the full course, even if you are feeling better.
- Be aware of rising rates of sexually-transmitted diseases—use protection and take precautions.
CRE infections are advancing across the country, causing an estimated 600 deaths per year. Unidentified to protect her privacy, the Nevada woman is now one of those numbers. As physicians and researchers work to create new drugs and develop alternative methods to fight resistant bacteria, those numbers are likely to go up, before they go down.
Just updated your iPhone? You'll find new emoji, enhanced security, podcast transcripts, Apple Cash virtual numbers, and other useful features. There are even new additions hidden within Safari. Find out what's new and changed on your iPhone with the iOS 17.4 update.





















Be the First to Comment
Share Your Thoughts