When the mosquito that carries the malaria parasite (Plasmodium falciparum) bites someone, the parasite must travel to the liver where it undergoes part of its lifecycle before infecting red blood cells and spreading to its next host. Until now, the first step of how the parasite gets to the liver hasn't been clear.
A group of researchers led by Dr. Justin Boddey, Dr. Sara Erickson, and Ms. Annie Yang, from the Division of Infection and Immunity at the Walter and Eliza Hall Institute in Victoria, Australia, just released new research in the journal Cell Reports detailing how the malaria parasite travels from the site of a mosquito bite into liver cells.

The researchers infected mice with human liver cells with malaria. They genetically engineered the parasite to lack certain components so they could figure out which ones were vital for entering into the liver cells.
They found that the parasites secrete two proteins, SPECT and PLP1, that stay on the parasite's surface and are needed for the parasite to be able to enter into a human cell. Without the ability to traverse into cells, the parasites couldn't get to the liver and establish an infection.
That critical step of cell transversal starts the cycle that results in a case of malaria, where the infected person feels the symptoms of the disease. And it may also be the target for stopping the disease.
"Our long-term goal is to eradicate malaria, so we have to look at ways of breaking the cycle of infection," Boddey said in a press release. "A vaccine or treatment that halts the liver-stage infection offers the best chance of eradication because it stops parasites before they take hold."
The Vicious Cycle
It all starts with a bite from an anopheles mosquito infected with the malaria parasite. Parasites in the sporozoite life stage are injected into humans from the insect bite.
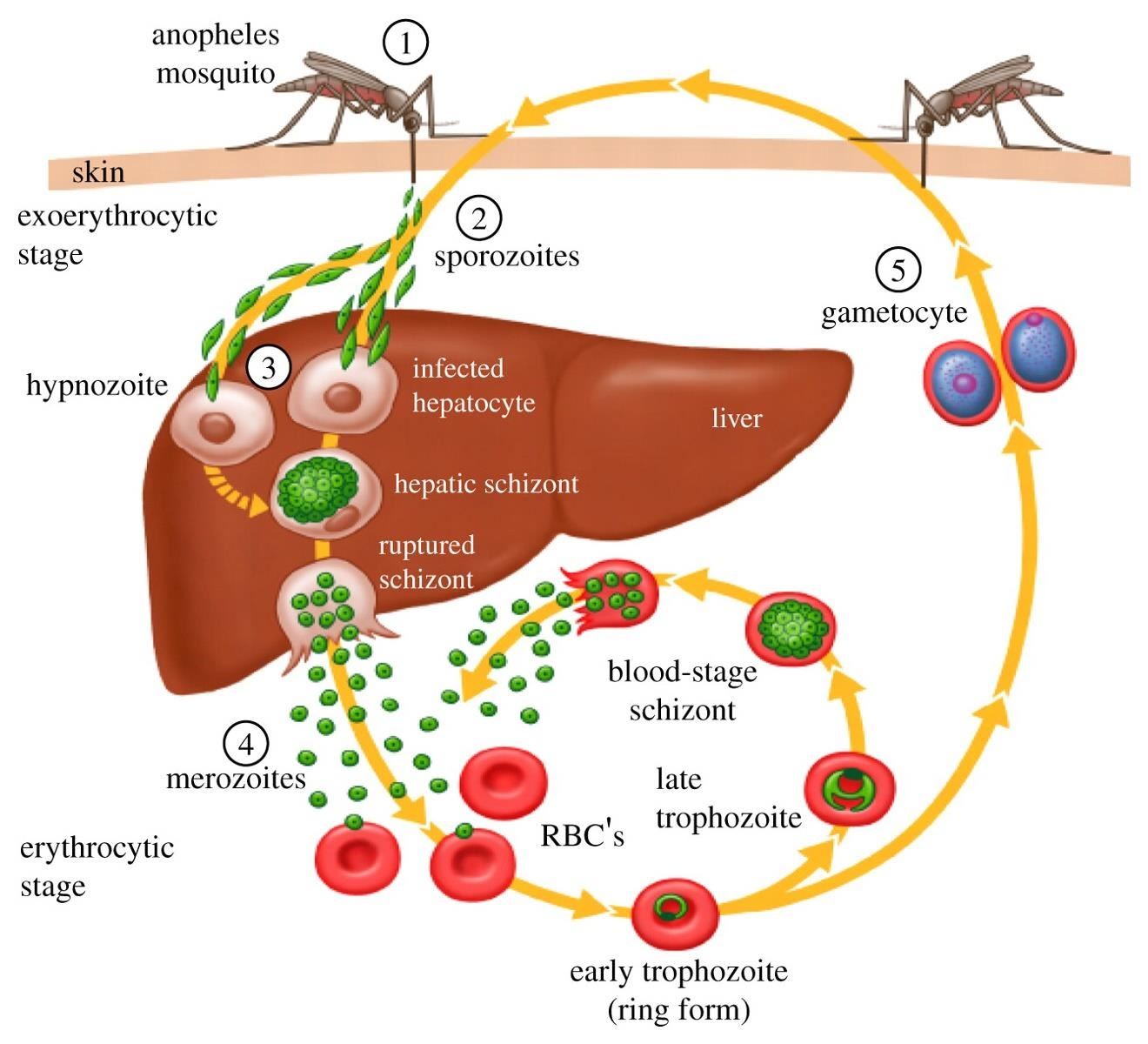
Thanks to the new research from Boddey and colleagues, we now know how the sporozoites transverse cells and make their way to the liver, where they infect the liver hepatocyte cells.
Once the merozoite stage of the parasite bursts from the infected liver cells, they infect red blood cells. This is the stage where symptoms of the infection occur. Malaria symptoms appear seven to 15 days after being bitten by an infected mosquito. The first symptoms are fever, headache, chills, and vomiting.
Malarial infections are treated with quinine-type medications (chloroquine, mefloquine, quinine, or quinidine), atovaquone-proguanil, or artemether-lumefantrine.
Once inside red blood cells, the parasite can develop through the trophozoite stage to the schizont stage, where they can burst the red cells, releasing particles that can infect more red cells. Mosquitos that feed on an infected person's blood during this stage pick up more of the parasite it can inject into other people. And the cycle continues in another victim.
The Global Threat of Malaria
Most cases of malaria occur in tropical and subtropical areas throughout the world. Although there are five types of malarial parasites, P. falciparum is the type responsible for most of the deaths.
In 2015, the World Health Organization estimated that there were 212 million people infected with malaria and 429,000 deaths. Seventy percent of the deaths occur in children under age five.
Despite concentrated research and health agency efforts to develop a malaria vaccine, effective anti-malarials, and insecticides, malaria remains a global health threat. The Centers for Disease Control and Prevention cite several reasons for this: an efficient mosquito that transmits the infection, a high prevalence of the most deadly species of the parasite, favorable climate, weak infrastructure to address the disease, and high intervention costs that are difficult to bear in poor countries.
If a good vaccine or treatment target could be found, like the mechanism involved in cell transversal, that might open up an opportunity to get ahead of this global health threat.
Just updated your iPhone? You'll find new emoji, enhanced security, podcast transcripts, Apple Cash virtual numbers, and other useful features. There are even new additions hidden within Safari. Find out what's new and changed on your iPhone with the iOS 17.4 update.





















Be the First to Comment
Share Your Thoughts